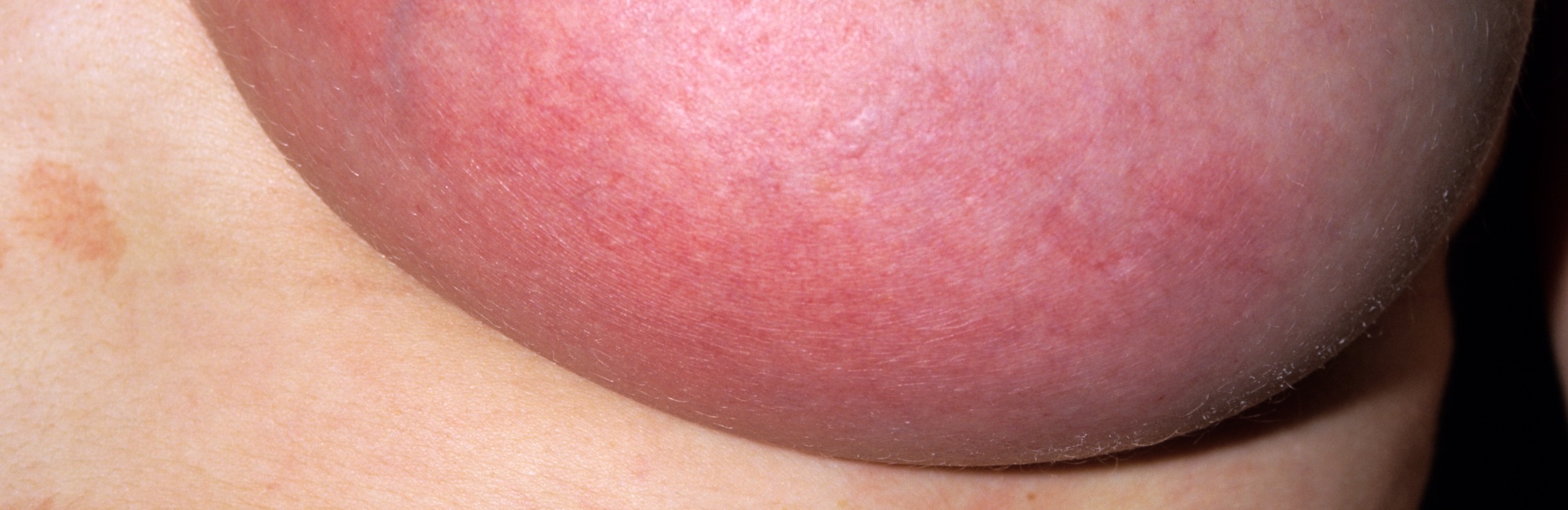
Why most women don't need to worry about overstimulating their breasts or removing too much milk when they have mastitis or breast inflammation

Historically women have been advised to offer the affected breast as often as a baby was interested if they had mastitis
Until the last few years in the West, breastfeeding women with mastitis were advised to
-
Offer the affected breast just as often as possible (without ever pressuring the baby)
-
Preference the affected breast (ensuring that the other breast doesn't overfull and also develop a mastitis).
This advice was built from personal and clinical experience. No-one ever researched it.
A short history of the belief that you mustn't overstimulate your breasts when you have mastitis
Then in the USA in particular, the idea took hold over the past decade that breast inflammation resulted from pathological bacteria and biofilms forming inside the ducts of the lactating breast. I watched as all the fascinating new information about the human milk microbiome began to be interpreted by various high profile breastfeeding doctors as a reason to think that mastitis was due to blockages in the ducts caused by bacteria and biofilms. For a while, everyone was advised to massage out the lumps. By the time the Academy of Breastfeeding Medicine's Clinical Protocol #36, The Mastitis Spectrum came out, the US-based doctors were no longer saying to massage out lumps. Instead, the new advice proposed that
-
There is always a normal biofilm lining all the milk ducts (a theory which I disputed in my own research publications) and that when this biofilm thickens and closes up the duct, we end up with mastitis
-
It is important not to increase frequency of milk removal from your breasts when you have mastitis.
Lately, the most popular theory proposed by US-based breastfeeding medicine doctors, who have global influence, has changed again, with a bigger focus now on the theory that high levels of lactose in the milk glands cause inflammation in the stromal tissues (another theory which doesn't hold up to research-based scrutiny). But the advice not to overstimulate the breasts by keeping frequency of milk removal the same as before you have mastitis, and offering breasts alternatively (rather than preferencing the affected one) has remained constant and is now embedded in most clinical guidelines for mastitis, including in Australia, despite lack of supporting evidence.
In the meantime, I've been trying to draw attention to our big health system blind spot about the importance of mechanical pressures in lactation, and also to the specific sociocultural context in the USA out of which the advice against overstimulation of the breasts has arisen, and which shouldn't be generalised. There are very high levels of exclusive pumping of breast milk in the USA, which does appear to result in high levels of oversupply, where more milk is being produced than the baby needs each day. But this is not such a prominent issue in countries which have lower levels of pumping.
The advice not to overstimulate your breasts if you have mastitis makes a number of assumptions which may not apply to you
Advise to both 'keep your milk flowing' at the same time as you 'avoid overstimulation' is not only confusing but actually quite stressful, because it's hard to know what this means! It seems to say that if you get it wrong, you'll continue to be sick and miserable with mastitis and it'll be your fault!
The advice not to overstimulate your breasts conflicts with some things that we know for sure about breastfeeding.
-
Advice not to overstimulate your breasts assums that you are exclusively or predominantly directly breastfeeding, your baby is unable to moderate his own caloric needs. That's not true! Once clinical problems have been sorted out, we can trust babies to self-regulate breastfeeding. If you offer the affected breast and your baby refuses, that's ok, since it's very important never to pressure your baby to feed. Sometimes, a woman might even hand express to keep the milk moving, if her baby is feeding less than usual during the mastitis, or she feels like it might be helpful. It makes the most sense from what the science tells us, even though it's not proven, to think that lots of letdowns in the affected breast helps resolve the inflammation.
-
Advice not to overstimulate your breasts assumes that your baby will quickly cause you to have high levels of milk, beyond her caloric needs. However, producing more milk than your baby needs, in a way that causes a problem for either you or your baby, is an occasional but not typical experience for breastfeeding women. This is proven by the fact that breastfeeding women all around the world report low supply as their main breastfeeding concern.
-
Advice not to overstimulate your breasts assums that is not spacing out feeds which has resulted in the mastitis, actually! Spacing out feeds, perhaps accidentally by having an unexpectedly long block of uninterrupted sleep overnight, is accepted as a cause of mastitis. Spacing out breastfeeds also commonly results in low supply. If you have a bounce in your supply due to offering the affected breast more often over a few days until the mastitis has resolved, this is not a bad thing! Low supply, even if temporary, appears to be a research-based outcome of mastitis (not high supply), and certainly I see this in some women after a severe mastitis. Any temporary increase in supply counters the tendency of mastitis to cause low supply! If we're using our breasts to feed baby frequently and flexibly, we don't need to be focussing on anything other than frequent offers on the affected side, in a way that protects the other side too.
If you are pumping your breast milk and have mastitis
Women who are pumping their milk will make judgement calls about how often to stimulate letdowns, and may decide not to increase the frequency of pumping if they are prone to levels of milk production beyond their baby's need.
However, it may also be that increased frequency of pumping on the affected side helps resolve the mastitis more quickly. Working out how best to proceed will depend on your own unique context.
Recommended resources
PBL Advanced
Why advice to NOT change patterns of breastfeeding when a woman has mastitis risks worsened outcomes
PBL Intermediate
A closer look at breast inflammation, fever, and use of anti-inflammatory medications
Probiotics (including Qiara) don't help prevent or treat breast inflammation
PBL Foundations
Why your letdowns help prevent or heal breast inflammation
When might you need antibiotics for mastitis?
How Jessie recovered from mastitis
Why lymphatic drainage and therapeutic massage don't help with breast inflammation
Selected references
Douglas P. Re-thinking benign inflammation of the lactating breast: a mechanobiological model. Women's Health. 2022;18:17455065221075907.
Douglas PS. Re-thinking benign inflammation of the lactating breast: classification, prevention, and management. Women's Health. 2022;18:17455057221091349.
Douglas PS. Does the Academy of Breastfeeding Medicine Clinical Protocol #36 'The Mastitis Spectrum' promote overtreatment and risk worsened outcomes for breastfeeding families? Commentary. International Breastfeeding Journal. 2023;18:Article no. 51 https://doi.org/10.1186/s13006-13023-00588-13008.